If you’re a woman with ADHD, there’s a decent chance you’ve had this thought at least once:
“Why the hell do I feel like a completely different person every couple of weeks?”
You’re not imagining it.
ADHD can already be a frustrating, exhausting experience—but for women, it often comes with an extra layer of complexity. Not only are women more likely to be diagnosed later (after years of wondering what’s “wrong” with them), but ADHD symptoms in women tend to fluctuate throughout the monthly hormonal cycle.
Which means just when you feel like you’ve finally gotten your life together… your brain is like, “Cool, let’s burn it down again.”
You’re Not Crazy, But Hormones + ADHD Will Make you feel that way sometimes
A lot of women I work with start to wonder if they might have something like bipolar disorder because their mood, focus, motivation, and emotional regulation seem to swing so dramatically.
Let me normalize this for you right now: That experience is incredibly common for women with ADHD.¹
What you’re likely noticing isn’t a personality flaw or a separate diagnosis—it’s the interaction between your ADHD and your hormonal cycle.
How the Menstrual Cycle Impacts ADHD Symptoms
Your menstrual cycle isn’t just about your period—it’s a full hormonal rhythm that affects your brain chemistry throughout the month, especially dopamine and serotonin, which are already involved in ADHD.²
Here’s a simplified breakdown:
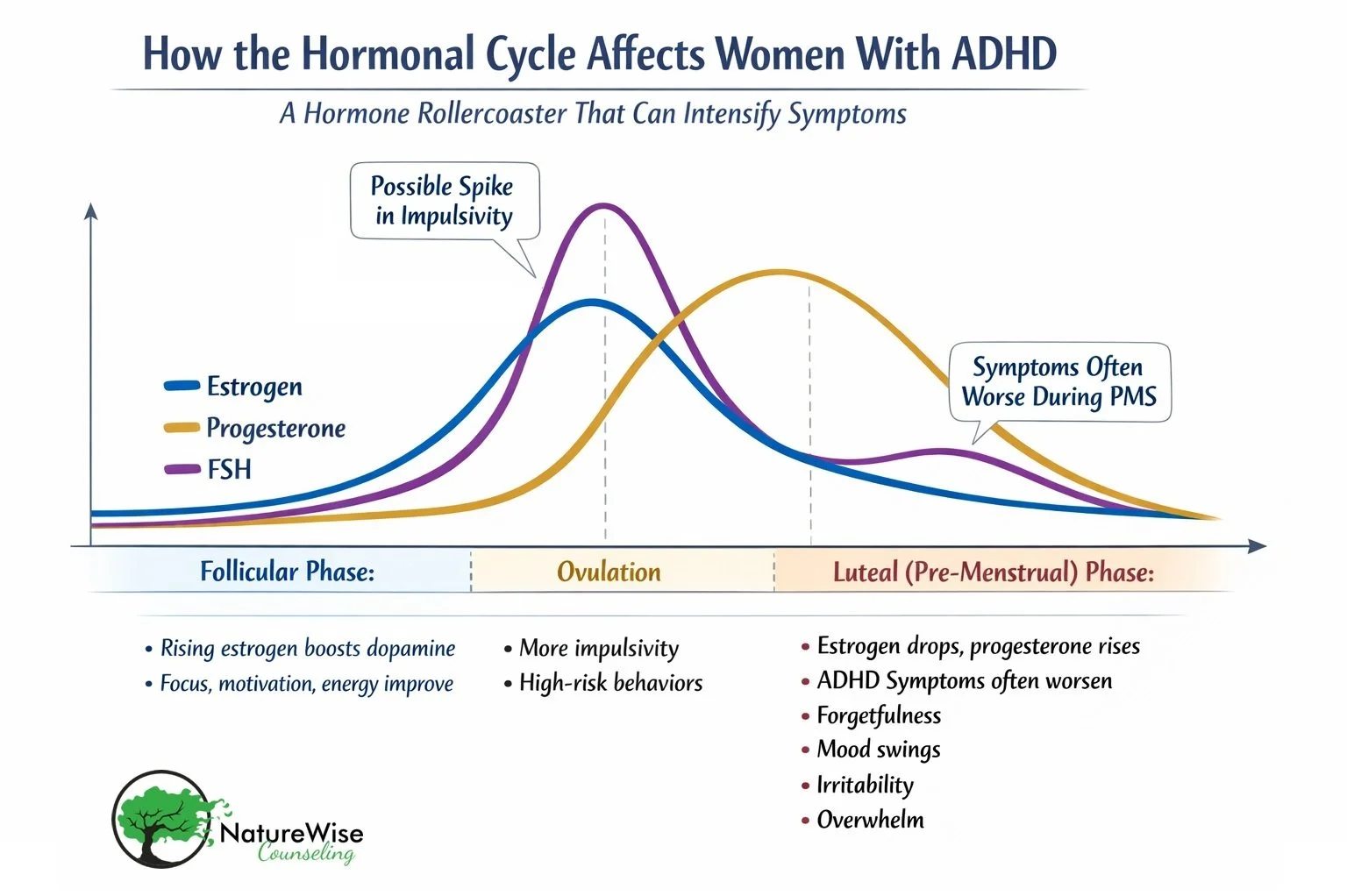
Follicular Phase (~Days 1-14: period + Shortly after)
Estrogen begins to rise → dopamine activity improves
You may feel more focused, motivated, and capable
This is often your “get stuff done” window—use it wisely.
Ovulation (~Day 14)
Estrogen peaks
Some women feel energized, social, and confident around this time
But for ADHD brains?
That boost can sometimes tip into impulsivity or risk-taking behaviors (hello, sudden “great ideas” with zero follow-through, or spontaneous sexual dalliances you later wonder about).
Luteal Phase (~Days 15-28: Pre-Menstrual / PMS)
Estrogen drops, progesterone rises → dopamine dips
This is where things can get rough
This is when ADHD symptoms often intensify:
Forgetfulness goes through the roof
Emotional regulation gets… spicy
Motivation disappears
Everything feels harder than you want it to
And then you might wonder:
“Why can’t I just get it together like I could last week?”
Because your brain chemistry literally changed.³
Why ADHD Symptoms Get Worse During PMS
During the pre-menstrual phase, lower estrogen means less dopamine support—aka the exact neurotransmitter ADHD brains already struggle with.
So yes—your ADHD symptoms can absolutely get worse during PMS.⁴
This can show up as:
Increased distractibility
Emotional overwhelm
Irritability (or rage, let’s be honest)
Low frustration tolerance
Women with ADHD and PMDD
Women with ADHD are also more likely to experience PMDD (Premenstrual Dysphoric Disorder)—a more severe version of PMS that includes significant mood disruption.⁵
Why?
Because ADHD already involves challenges with emotional regulation, and when hormones amplify that… it can hit hard.
Pregnancy, Postpartum, and ADHD
Hormonal shifts don’t stop with your monthly cycle.
Pregnancy and postpartum can intensify ADHD symptoms, especially with sleep disruption, identity shifts, and massive hormonal changes.⁶
Many women notice:
Increased brain fog
Difficulty organizing or planning
Heightened emotional sensitivity
A Quick Note on Perimenopause
If this feels like a lot… just wait until perimenopause enters the chat.
(Just kidding… sort of.)
I’ll be covering that in next week’s blog, because it deserves its own deep dive.
Why Figuring out if it’s ADHD is So Frustrating for Women
Because your symptoms are constantly shifting, ADHD in women can look inconsistent—and that can lead to:
Misdiagnosis
Being dismissed
Internalizing shame (“Why can’t I just get it together?”)
But the truth is:
Your ADHD isn’t inconsistent—your hormones are just changing the playing field every couple weeks.
What You Can Do to Cope
You’re not powerless here. A few strategies can make a huge difference:
1. Track Your Cycle
Start noticing patterns. When are you focused? When are you struggling?
Awareness = power.
2. Talk to Your Prescriber
If you take medication, some women benefit from adjusting stimulant dosage during certain phases.⁷
3. Adjust Your Schedule
Plan demanding tasks during higher-energy phases
Lower expectations during PMS weeks
Build in more support when you know you’ll need it
4. Practice Self-Compassion (Seriously)
You’re not lazy—you’re navigating a shifting neurochemical landscape. So go easy on yourself.
You Don’t Have to White-Knuckle This alone
Working with an ADHD therapist or coach who actually understands this interplay can be a game-changer.
If you want support navigating the ups and downs of your cycle and your ADHD, you can learn more about how I work with ADHD and see if therapy or coaching might help you.
I bring both professional training and lived experience into this work—and I promise, you won’t have to explain to me why this is hard. I get it.
Let’s Figure This Out Together
If this is hitting a little too close to home, you’re not alone—and you don’t have to keep guessing your way through it.
I offer free consult calls where we can talk through what you’re experiencing and make a plan that actually works for your brain.
References
Quinn, P. O. (2005). Treating adolescent girls and women with ADHD
Volkow, N. D. et al. (2009). Dopamine and ADHD
Jacobs & Goldstein (2018). Estrogen and cognitive function
Rucklidge, J. J. (2010). Gender differences in ADHD
Epperson, C. N. et al. (2012). Premenstrual dysphoric disorder
Anderson, K. N. et al. (2018). ADHD in pregnancy and postpartum
MGH Center for Women’s Mental Health (clinical guidance)